20
Mammography images are created by the process of x-rays passing through breast tissue and interacting with a digital detector. The anode in the x-ray tube used for mammography is made of molybdenum, or rhodium, rather than tungsten which is commonly used in general x-ray tubes. For more information about x-ray formation see the previous section (X-rays).
This physical change to the x-ray tube anode results in a different spectrum of x-rays that are better suited to assessing the fat, connective tissue, and mammary tissue found in the breast. This allows for very detailed images of soft tissues using x-rays as the source of radiation. This imaging modality is predominantly used to image the female breast tissue but it is also capable of imaging male breast tissue for assessment of a palpable nodule or mass. A standard, digital, mammography unit is seen in Figure 3.12.
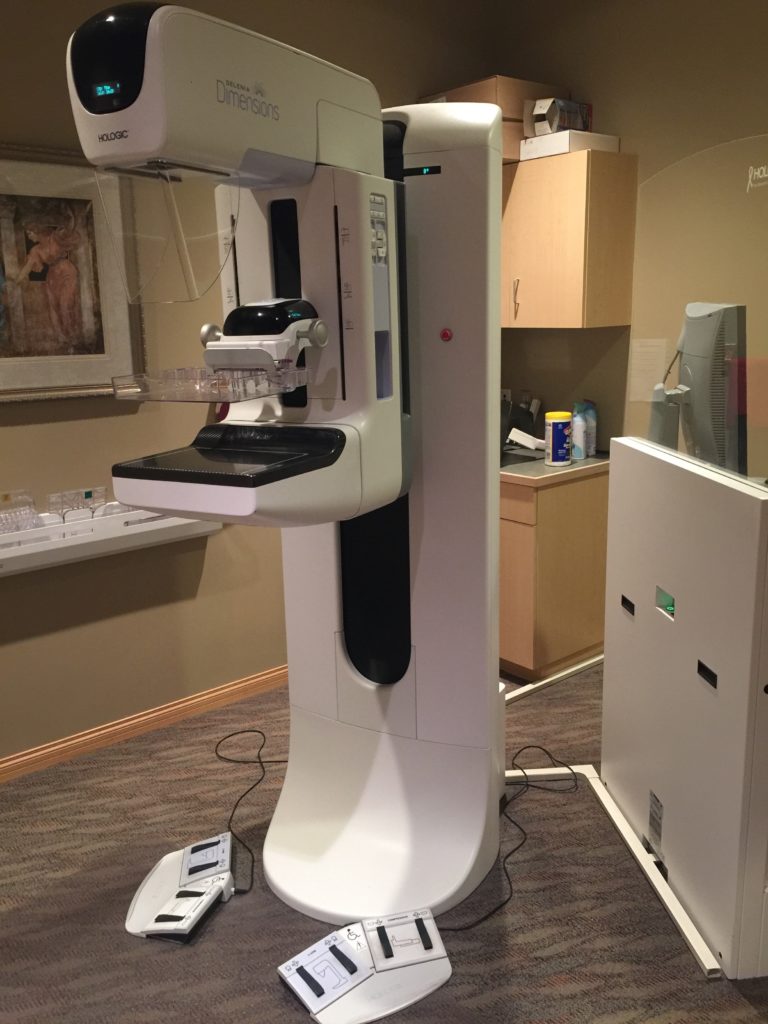
The standard positions for image acquisition in mammography is the cranial-caudal view and an oblique view. Additional mammographic positions, such as the lateral view, are used to problem solve complex abnormalities. The mammographic x-ray tube and detector are able to rotate along the coronal axis of the machine to allow for image acquisition in various planes to maintain stable patient positioning without the need for the patient to lean or tip in any particular direction. Newer mammography machines routinely obtain images as the x-ray tube and the detector plate rotate resulting in a process called tomosynthesis.
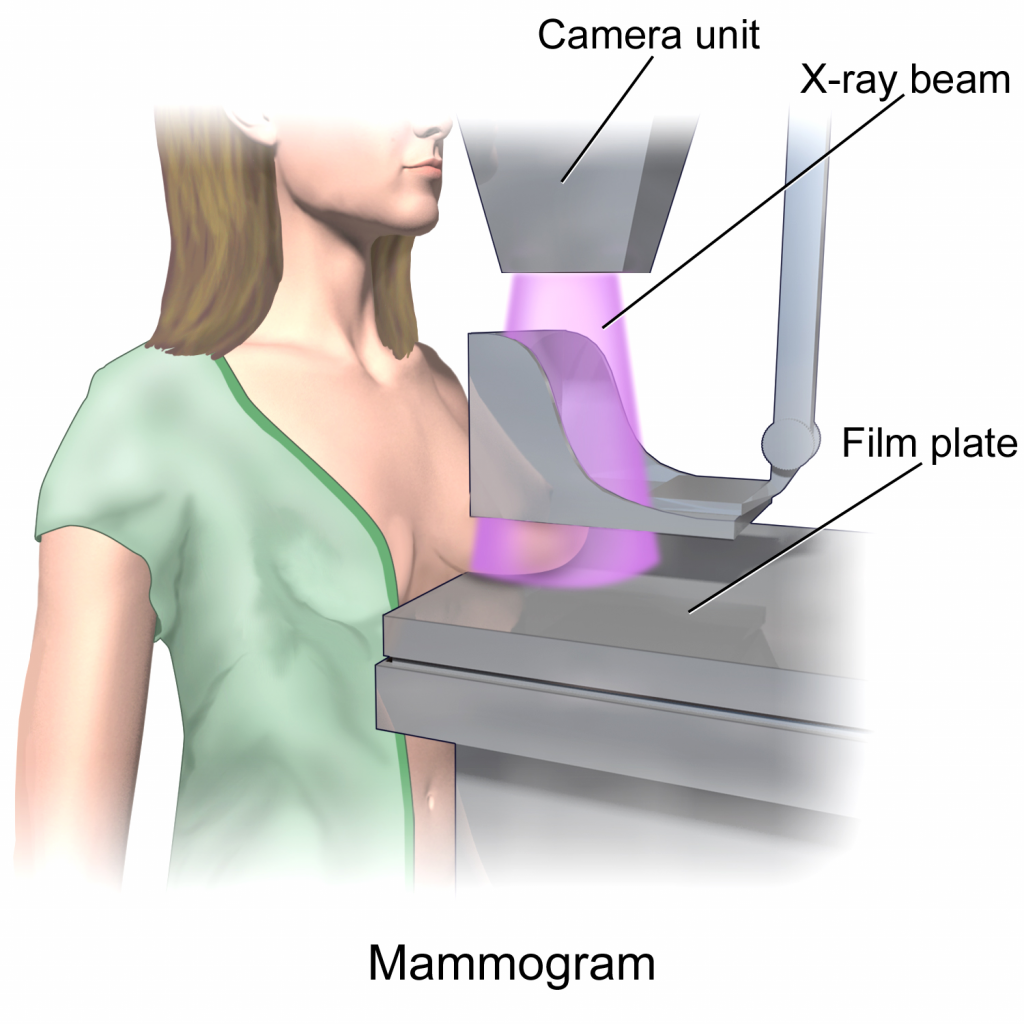
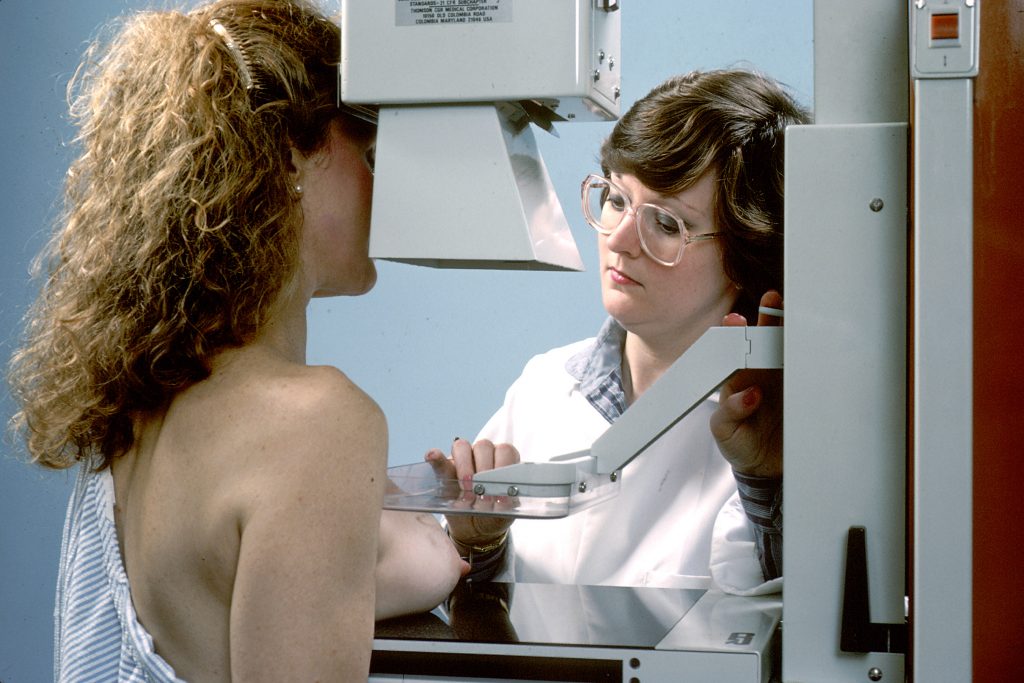
In order to minimize x-ray scatter and create a relatively uniform tissue density prior to x-ray exposure of the breast tissue it is standard practice to compress the breast tissue between radiolucent plastic plates. This can be uncomfortable for some patients but it is not dangerous or overly painful. An image of a patient positioned for a cranial-caudal mammographic image is provided (Figure 3.13).
The same general concepts of appearance of different tissues on x-rays applies to mammography, i.e. air is black, fat is lower opacity than mammary glands and connective tissue and calcium is the most opaque element visualized. The detection of small calcifications is a common finding on mammograms depicting breast cancer. The resulting x-rays generated by mammography are seen in Figure 3.14.
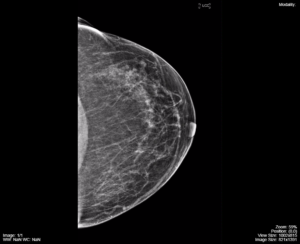
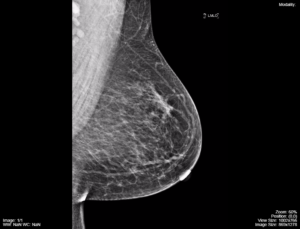
These screening images depict normal breast tissue, fat, and connective tissue. The more opaque tissue at the back edge of the images is the pectoralis major muscle. The breast tissue is predominantly fat replaced and there is no evidence of atypical calcifications, a nodule, mass, or architectural distortion. Normal lymph nodes are seen in the axillary area.
Attributions
Fig 3.12 Mammography x-ray Machine by Dr. Brent Burbridge MD, FRCPC, University Medical Imaging Consultants, College of Medicine, University of Saskatchewan is used under a CC-BY-NC-SA 4.0 license
Fig 3.13A Illustration for positioning for a Cranial-Caudal (CC) Mammogram by Bruce Blausen. Used under Creative Commons Atribution CC BY, 3.0, Unported. https://en.wikipedia.org/wiki/Mammography#/media/File:Blausen_0628_Mammogram.png
Fig 3.13B Imaging of a patient being positioned for a CC Mammogram. National Cancer Institute, Bill Branson. This image is in the public domain and can be freely reused. cancergovstaff@mail.nih.gov
Fig 3.14A Mammography CC image, left side, normal screening mammography image by Dr. Brent Burbridge MD, FRCPC, University Medical Imaging Consultants, College of Medicine, University of Saskatchewan is used under a CC-BY-NC-SA 4.0 license. Can be accessed from https://mistr.usask.ca/odin/?caseID=20170410101815189
Fig 3.14B Mammography, MLO image, left side, normal screening mammography image by Dr. Brent Burbridge MD, FRCPC, University Medical Imaging Consultants, College of Medicine, University of Saskatchewan is used under a CC-BY-NC-SA 4.0 license. Can be accessed from https://mistr.usask.ca/odin/?caseID=20170410101815189
